The Best Breastfeeding Positions (And How to Find the One That Actually Works for YOU)
One of the biggest myths about breastfeeding is that there’s one “right” way to hold your baby.
You know the image: perfectly upright parent, classic cradle hold, tiny peaceful baby, soft lighting, nobody sweating.
Meanwhile in real life? You’re balancing a hungry newborn, trying not to aggravate your stitches, wondering why your neck hurts, and questioning whether babies are secretly born with octopus arms.
Here’s the truth: there is no gold medal breastfeeding position.
The best feeding position is the one that helps your baby transfer milk well, feels sustainable for your body, supports a deep latch, and doesn’t make you dread the next feeding.
Different seasons, different babies, and different postpartum recoveries often call for different positions too. What works on day 2 may not be your favorite at 6 weeks. Let’s walk through the most common positions — plus when each one can be especially helpful.
Cradle Hold
This is the classic position most people picture when they think about breastfeeding. Baby lays across your body tummy-to-tummy with their head resting in the crook of your arm on the same side as the nursing breast.
Why parents like it:
• Feels intuitive once feeding is established
• Easy for feeding in public
• Comfortable for older babies with better head control
One thing to know: for brand new babies, cradle hold can sometimes make it harder to guide the latch because the arm supporting baby has less control over head positioning. A lot of parents are placed in cradle hold immediately after birth — before anyone has walked them through latch mechanics — and end up assuming breastfeeding is supposed to hurt. It isn’t.
Cross-Cradle Hold
Think of this as cradle hold’s more supportive cousin. Instead of supporting baby with the arm on the same side as the nursing breast, you use the opposite arm. This gives you significantly more control over baby’s head during latch-on.
Why IBCLCs love this one:
• Great for learning latch mechanics
• Helpful for newborns and early days
• Allows more precise positioning adjustments
• Makes it easier to correct a shallow latch before it causes damage
This is often the position where one small adjustment changes everything.
Football Hold
Baby tucks alongside your body under your arm, with their legs pointing behind you toward your back — toes touching your spine. This tucked position helps keep baby stable and well-supported throughout the feed.
This position can be a game changer for:
• Cesarean recovery — keeps baby off your incision
• Larger breasts
• Twins
• Parents who want better visibility during latch
Pro tip: line up the nipple to baby’s nose so that baby has to reach slightly for the nipple. This naturally encourages an asymmetrical latch — meaning baby takes more breast tissue on the chin side than the nose side. That off-center latch is actually what you’re going for, and it applies to every position. A centered latch is almost always a shallower latch.
And as always — bring baby TO you. Do not spend an entire feeding leaning your body down toward baby. That’s a fast track to neck and upper back pain on top of everything else you’re already recovering from.
Side-Lying Feeding
This one is my personal favorite — and after nearly 14 years as an IBCLC, I’ve tried them all.
Side-lying allows you to nurse while lying on your side with baby facing you tummy-to-tummy. And I genuinely believe it is one of the most underused positions in the early weeks.
Before breastfeeding chairs and nursing pillows existed, moms fed their babies lying down. In many cultures today, new mothers stay in bed or close to bed for the first 30 to 40 days after birth. There’s a reason for that. Rest and proximity to baby are not luxuries. They are medicine.
Here’s why I reach for this position clinically: babies can almost always get a deeper latch in side-lying. And when a mom has a sore belly from a cesarean, fresh stitches from a perineal repair, a baby who has been cluster feeding for three hours, or a body that is simply done sitting upright — side-lying changes everything.
To set it up:
• Lie on your side with baby tummy-to-tummy
• Line the nipple up to baby’s nose — baby should have to reach slightly for the breast, which encourages that deeper asymmetrical latch
• Roll baby in close rather than leaning your breast down toward them
• A pillow behind your back and between your legs makes a world of difference for comfort
You’re looking for a wide open mouth, chin touching breast, deep asymmetrical latch, and swallowing sounds once milk is flowing.
One important note: if there is any chance you might fall asleep, have another adult nearby to supervise. For families who want to learn more about safer sleep practices, this is something we’re happy to talk through during a consult.
When I help a mom get comfortable in side-lying, she almost always says the same thing afterward: “Why did nobody tell me about this sooner?”
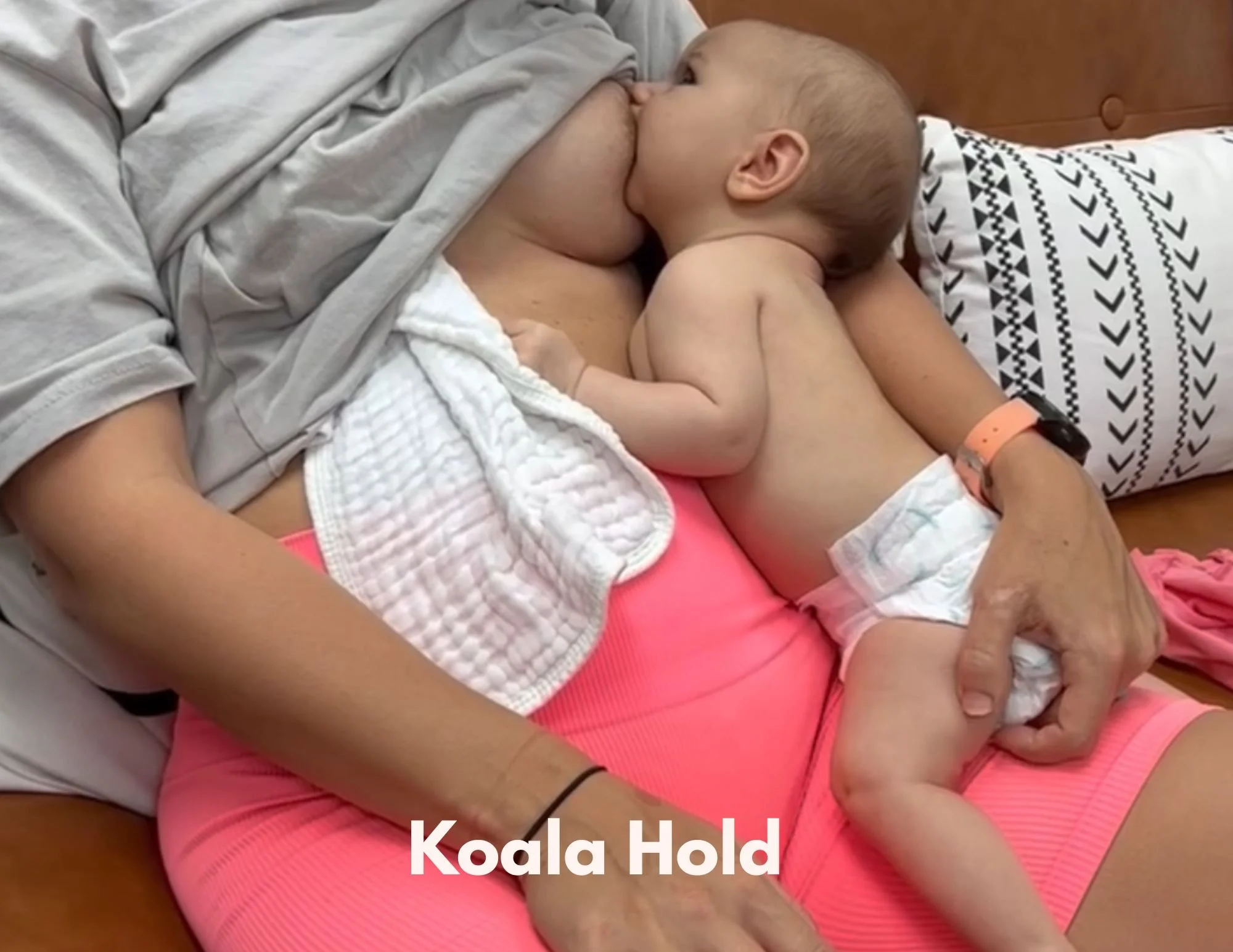
Koala Hold
The koala hold — sometimes called the upright or straddle hold — has baby sitting straddled upright on your thigh or hip, facing your breast with their spine vertical.
This position is especially helpful for:
• Babies with reflux or who spit up frequently — gravity works in their favor when they’re upright
• Babies with ear infections — horizontal feeding can be uncomfortable
• Older babies with strong head and trunk control who prefer to sit up
• Fast letdown or overactive milk ejection reflex — the upright angle helps baby manage flow more easily
• Babies who consistently pull off or seem overwhelmed during letdown
The latch mechanics are the same: nipple to nose, baby reaches up slightly for the breast, and you’re aiming for that deep asymmetrical latch with chin in first.
Laid-Back Feeding (Biological Nurturing)
In this position, the parent reclines comfortably while baby lays on top of the chest or torso. This works with newborn reflexes instead of against them and can be surprisingly effective for families who are struggling.
This is my other personal favorite — and for good reason. When a baby is draped across your body with gravity doing the work, feeding often just clicks in a way it doesn’t in other positions. It slows everything down. It brings you both back to basics.
Especially helpful for:
• Fast letdown or oversupply
• Babies who are overwhelmed by milk flow
• Skin-to-skin time
• Encouraging instinctive feeding behaviors
• Parents who want a more relaxed, low-effort setup
Gravity does a lot of the work here — slowing the flow and helping baby pace themselves.
So Which Position Is Best?
Honestly? The one that works for you and your baby right now.
But if you’re asking for my personal favorites after nearly 14 years of doing this — side-lying and laid-back feeding win every time. They are the two positions that consistently unlock deeper latches, give exhausted moms permission to actually rest, and make the early weeks feel more survivable. I will never stop talking about them.
The best position overall is the one that allows a deep comfortable latch, effective milk transfer, less nipple pain, sustainable feeding sessions, and less tension in your body. And that answer may change throughout your entire breastfeeding journey. Many parents rotate through multiple positions depending on baby’s mood, milk flow, where they’re feeding, and how exhausted they are that day.
A Quick Note About Pain
A new position can feel awkward at first — that’s normal. But sharp pain, pinching, nipple damage, or curling your toes through an entire feed are signs that something needs adjusting. Tiny positioning changes can make a huge difference in both comfort and milk transfer. If feeding hurts, that is information — not a character flaw.
You Don’t Have to Figure This Out Alone
One of the most common things we hear during consults is: “I wish someone had shown me this sooner.”
Sometimes a single position tweak completely changes feeding. During a lactation consult, we can help you troubleshoot painful feeds, find positions that work for your specific body and baby, improve latch and milk transfer, adapt positioning after a cesarean, and work through reflux, fast letdown, oversupply, or sleepy feeding.
Because breastfeeding should not feel like an endurance sport.
My team of IBCLCs serves families across the entire Phoenix Valley — in your home and in our offices — and via telehealth anywhere in the United States. Most visits are covered by insurance.
Click here to check your coverage and book with my team: https://www.azbreastfedbabies.com/appointments
I’m Amey Fields, RN IBCLC — an 18-year labor and delivery nurse and board-certified lactation consultant. I own AZ Breastfed Babies, a team of 18 IBCLCs supporting families across the Phoenix Valley and nationwide via telehealth. I am an IBCLC but not YOUR IBCLC (yet 🧡). Information shared here is not individualized advice. Personalized guidance is provided through one-on-one consults only.